Uveitis
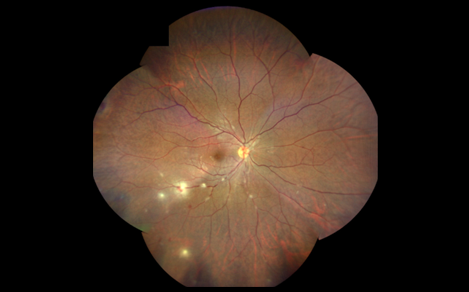
What is Uveitis?
What causes Uveitis?
Types of Uveitis
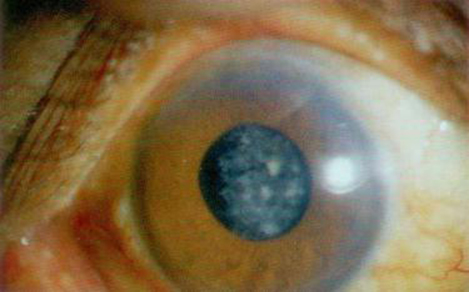
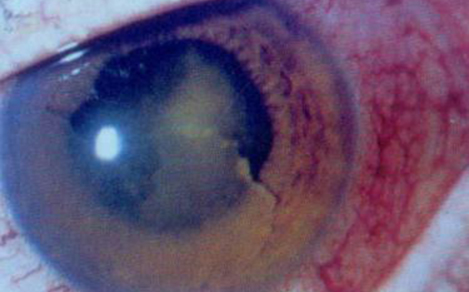
Anterior Uveitis: This kind of Uveitis affects the front or anterior portion of the eye. The common symptoms are redness, watering, decreased vision, pain in the eye, and photophobia or intense discomfort while looking at light. In low-grade inflammation, the eye may appear normal but still have s1gns of damage.
Intermediate Uveitis: In this type of Uveitis, the uveal tract (middle part of the middle layer) is affected. The patient usually sees black spots in front of the eye. There may be loss of vision due to fluid accumulation in the central area of the retina.
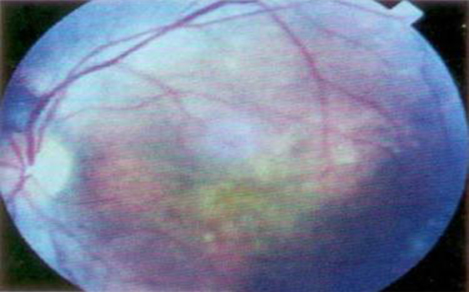
Posterior Uveitis: This type affects the back or the posterior portion of the eye. The eye may appear normal or there may be little inflammation in the front. The inflammation may affect the retina, choroid (posterior or back part of the middle layer) or both. The inflammation may be localised at several places, or even widely spread. Patients usually complain of poor vision, or absence of central vision or peripheral vision.
Panuveitis: Panuveitis affects the entire uveal tract (middle layer from the front and back). It often causes a distinct blurring of the vision with varying degrees of pain and redness. This is also associated with inflammation in the vitreous cavity at the back of the eye.